Operations on the mitral valve
Content: |
Department of Thoracic and Cardiovascular Surgery Homburg/Saar |
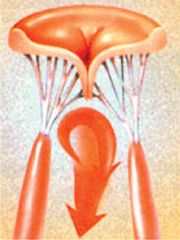
The mitral valve is the inlet valve of the left ventricle, which is the main pumping chamber of the heart and circulation. The valve should open fully during filling of the ventricle and should thus not generate resistance to the blood flow. When the left ventricle ejects blood the mitral valve should be completely competent and not allow leakage into the left forechamber. Inadequate opening is called Stenosis, incomplete closure or leakage during the ejection phase is called regurgitation..
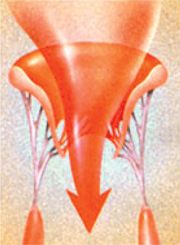 |  |
Stenosis of the mitral valve leads to insufficient blood supply of the body during exercise, alternatively it may result in increased pressure in the lung arteries. With increasing severity of the Stenosis and time that the valve has functioned inadequately high pressure and resistance may persist in the lung despite correction of Stenosis by an operation.
Leakage (regurgitation) poses a volume load to the left ventricle through the blood that flows backward during every ejection. This leads to enlargement of the left ventricle and increased amount of heart muscle, later also to decreased force that the heart muscle can generate during ejection of blood. The consequence will be insufficient blood supply of the body during exercise or increased pressure in the lung arteries. Damage of the heart muscle may ensue as well as irregular heart rhythm (atrial fibrillation).
Both forms of functional problems may be tolerated over years, and the patient feels little of his heart valve problem. Once certain thresholds have been reached there is an increased risk of dying from the complications of the mitral valve disease. It is the goal of the operation to correct the valve problem in order to avoid an increased risk before irreversible changes have occurred in the heart muscle or lung arteries. Typical signs are: decreasing exercise tolerance, increasing fatigue or shortness of breath, or chest pain. There are also specific changes that can be determined by an ultrasound study of the heart, such as decreased pumping force or marked enlargement of the left ventricle. Your physician can best judge which of these symptoms is most important in your situation.
The ideal solution would restore valve function fort he rest of the life and not have side effects. Unfortunately we do not yet have this ideal valve operation. There are several different possibilities. Each possibility has specific advantages and disadvantages, and we will need to find the best solution for your specific situation. You will find a summary of all possibilities even though not all may be reasonable in your specific case.
Mechanical valve replacement

Mechanical valves of current design were developed in the 1970s. They are made out of carbon (graphite) that changes its properties under high pressure and high temperatures and becomes a hard and durable material. This carbon is currently the best synthetic material for heart valves but still not ideal.
The durability of these valves is probably more than 40 years. On the other hand blood clots may form on the foreign surface of the valve, and these blood clots may be dislodged into blood vessels of the body or brain, or they may even block the valve. In order to minimize the formation of blood clots it is necessary to take medication that blocks the coagulation system of the blood, and this medication has to be taken lifelong (Coumadin, warfarin). The most important side effect of these drugs is the occurrence of bleeding problems that may happen as a consequence of trauma or even without a trauma. It is important and necessary to monitor the effect of the “blood thinners” carefully in order to keep the combined possibility of clot formation and bleeding problems at a minimum. With careful surveillance the risk of developing either a clot or a bleeding problem is in the range of 3 to 3.5% per year.
In certain situations (e.g. major dental procedures) bacteria may get into the blood stream, settle on the artificial heart valve, and cause a bacterial infection of the valve (so-called endocarditis). The likelihood of developing an endocarditis is approximately 1% per year, and these serious complications not only requires aggressive treatment with antibiotics, but also repeat replacement of the valve in an operation. Blockage of the valve is rare but also has to be treated by a repeat operation. Looking at a period of 15 years, the probability of valve-related complications is approximately 4 to 5% per year, and the likelihood of a second operation is 1% per year.
Biologic valve replacement
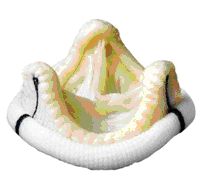
Biologic heart valves have existed since the 1970s. They are either specially prepared aortic valves of pigs or they are made out of pericardial tissue of cows. The animal tissue is prepared in such a way that it can be stored for years and maintains its form and function after implantation into the human body for as many years as possible. This preservation treatment also makes it unrecognizable as foreign tissue to the human body, so it cannot be rejected (as would happen if normal tissue or organs are implanted / transplanted). Therefore it is not necessary to take anti-rejection medication (immunosuppression).
Most biologic heart valves are mounted onto stents that stabilize their form and make implantation easy. More than 10 years ago so-called stentless heart valves were developed. They have a slight advantage in valve function, but it is still uncertain whether their durability is better than that of conventional biologic valves.
The tendency to develop clot formation with biologic valves is low, and treatment with specific blood thinners is recommended for only 3 months as long as heart rhythm is stable. Some cardiologists and cardiac surgeons recommend life-long intake of low-dose aspirin (100 mg per day) in order to keep the likelihood of clot formation low. Blockage of the valve with clots does not occur, the risk of bacterial infection (endocarditis) is identical to that of mechanical valves (appr. 1% per year).
The durability of biologic valves is principally limited because of degeneration (wear) of the valves. The time until the valve wears out is related to the age of the patient and increases with age. In young patients (<25 years) the mean durability is 5 to 7 years, in a 50 year-old about 8 to 10 years, and in a 70 year-old more than 20 years. When the valve is worn out a repeat operation or intervention is necessary. In the future a catheter-based intervention may be an alternative to a typical operation. The risk of a repeat operation depends on individual risk factors; in general it is only slightly higher than that of the first valve operation.
Looking at a period of 15 years the risk of valve-related complications in a middle-age patient (55 to 60 years) is about 4 to 5% per year with degeneration as the most important complication. Your physician can give you a personalized estimate.
Reconstruction of the mitral valve
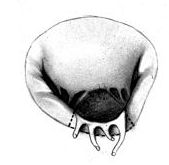 | 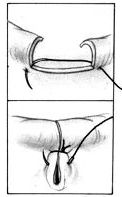 | 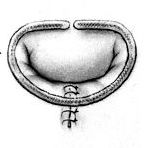 |
posterior mitral lealet with torn chords | reconstructed mitral valve |
This alternative to replacement of the mitral valve is the preferred option whenever possible, particularly in regurgitant mitral valves. Reconstruction is not always the same, since it has to address the individual characteristics of the regurgitant mitral valve. Enlargement of the ring of the mitral valve (border between atrium and ventricle) has to be corrected. In most instances this will involve insertion of a prosthetic ring. Instability of one or both mitral leaflets will have to be corrected by insertion of artificial chords or resection of the unstable leaflet parts. Tissue defects are commonly corrected by insertion of patch material. By now there are also operative techniques that can correct a deformation of the left ventricle as the primary cause of mitral leakage. Your physician will be able to explain the individual defects of the mitral valve as well as the possibility and required techniques of repair. This is best done when the video of a transesophageal echocardiogram is available. The final decision will have to be made in the operating room after looking at the valve directly.
After reconstruction of the aortic valve the possibility of clot formation is minimal. We recommend Aspirin (100 mg per day) for the first 2 months postoperatively, later no blood thinners are necessary for the valve. Blockage of the valve with clot does not occur. The risk of bacterial infection (endocarditis) is lower than that after implantation of a mechanical or biological prosthesis (approximately 0,2% per year). In addition, repair has the advantage of having a lower risk of operation compared to replacement.
The durability of the reconstructed valve depends on its form (anatomy) and specific details that are found at the time of operation. Especially in young patients the stability is usually longer than that of a biological prosthesis, sometimes even better than the likelihood of reoperation after implantation of a mechanical valve. The likelihood of valve-related complications over a 10 to 15 year period is less than 2% per year. The most important event would be recurrence of the leak.
Conclusion
In conclusion, there is no ideal solution (yet). It is therefore important to find the best compromise for your problem. Reconstruction has an advantage over replacement due to 1. lower operative risk, and 2. fewer problems long term. The mechanical solution will be stable long term, but there are the problems of clot formation and blood thinners. The biological prosthesis will cause relatively few problems while it works, but the durability is limited. Reconstruction is thus the preferred approach whenever feasible. Unfortunately no treatment is free from the risk of a repeat operation, and the time to the next operation is difficult to predict for the individual.
You should carefully consider all information and make certain that all questions are answered. You also have to know that unforeseeable information found during the operation may lead to a change in plan. This is particularly relevant for the Ross operation and reconstruction. In order to allow the surgeon to make the best decisions for you you should define a procedure of choice (plan A) and a “second best” (plan B).
Prof. Dr. med. H.-J. Schäfers, 04.01.2019





